On April 28, 2021, Ellen Kelsay, President and CEO of Business Group on Health, testified before the U.S. House of Representatives Ways and Means Health Subcommittee on the present and future role of telehealth in the health care arena. Representing more than 55 million employees, retirees and their families in the U.S, Business Group members have long been at the forefront of adopting innovative benefit designs, with telehealth and increased access to mental health services among their top priorities. The Business Group ‘s long-term commitment to high-quality, cost-effective health care has given the organization an influential seat at the policymaking table.
Even before the COVID-19 pandemic, more than 90% of Business Group members were already offering some form of telehealth through their group health plans. The pandemic accelerated the process; according to Kelsay, “it is hard to overstate the effects of the COVID-19 pandemic on virtual care and telehealth adoption among employees, employers and providers.” The Business Group’s most recent survey illustrates this point: In 2020, 78% of employers saw greater utilization of virtual care solutions, and 67% increased access to telehealth visits for primary care services.
Business Group members also think that these changes are here to stay. Between 2018 and 2020, the percentage of members believing that virtual care will have a significant impact on how health care is delivered increased from an already robust 52% to 80%.
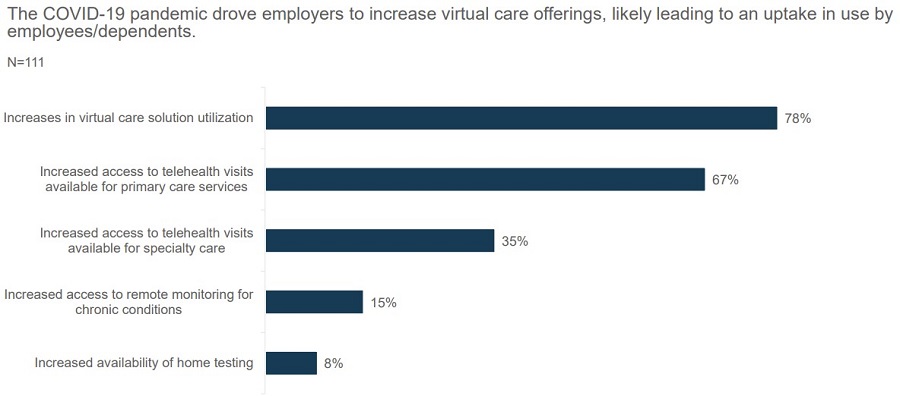
Source: 2021 Large Employers’ Health Care Strategy and Plan Design Survey
But there is still room for improvement. Although the pandemic spurred greater utilization of telehealth, resulting in an increase from 1% in 2019 to 30% in the first half of 2020, the median utilization rate is only 5%. This finding points to the potential for greater use of telehealth services, as well as careful monitoring of the long-term costs and impact on quality of care.
To address these concerns the Business Group believes that rigorous study of the following issues is needed:
- How health outcomes and the patient experience differ in in virtual and in-person settings;
- How telehealth can complement, not duplicate, in-person care; and
- How both the government and businesses can work together to ensure that virtual care and telehealth are uniformly available—and of uniform quality—nationwide.
Congress and regulatory bodies have a unique role to play in expanding access to telehealth services. During the pandemic, some steps were taken that the Business Group feels strongly should be made permanent policy. Other steps are long overdue:
- Permitting interstate licensure of providers; permitting telephone-only service when medically appropriate; and encouraging a national framework for telehealth for multistate employers as ways to expand and maintain equitable access to key services.
- Permanently allowing employees enrolled in employer-sponsored high-deductible health plans paired with health savings account to take advantage of virtual care and telehealth services, another way to ensure equitable access.
- Permanently offering virtual care and telehealth services to employees not enrolled in an employer’s group health plan, a strategy that will bring these services to more employees and their families.
- Conducting large-scale independent studies and analyses of health outcomes and costs, which the government is equipped to handle.
- Extending telehealth to the Medicare system, as was authorized in response to the COVID-19 pandemic, which would result in data to evaluate the costs and benefits of widespread availability.
