November 29, 2022
Note: This resource is intended to be useful both as a standalone document, as well as the fifth part of Business Group on Health’s Value-Based Purchasing Guide. Click the link to access additional parts related to other elements of employer value-based purchasing strategy.
Centers of Excellence (COE) are groups of providers who are selected to perform certain specialized services because of their expertise, favorable outcomes and, often, willingness to take on value-based payments. They are a common way for employers and health plans to incorporate value- based purchasing into their health care strategy for specific conditions and procedures.
This part focuses on the value-based care aspects of COEs. If you would like to learn more about how to assess COE opportunities, contracting strategies and more, the Business Group’s resource Centers of Excellence Considerations for Employers goes into much greater detail.
How Prevalent Are COEs?
According to the Business Group’s 2023 Health Care Strategy and Plan Design Survey, the vast majority of large employer respondents offer access to at least one type of COE; most rely on their carriers to set up these contracts.
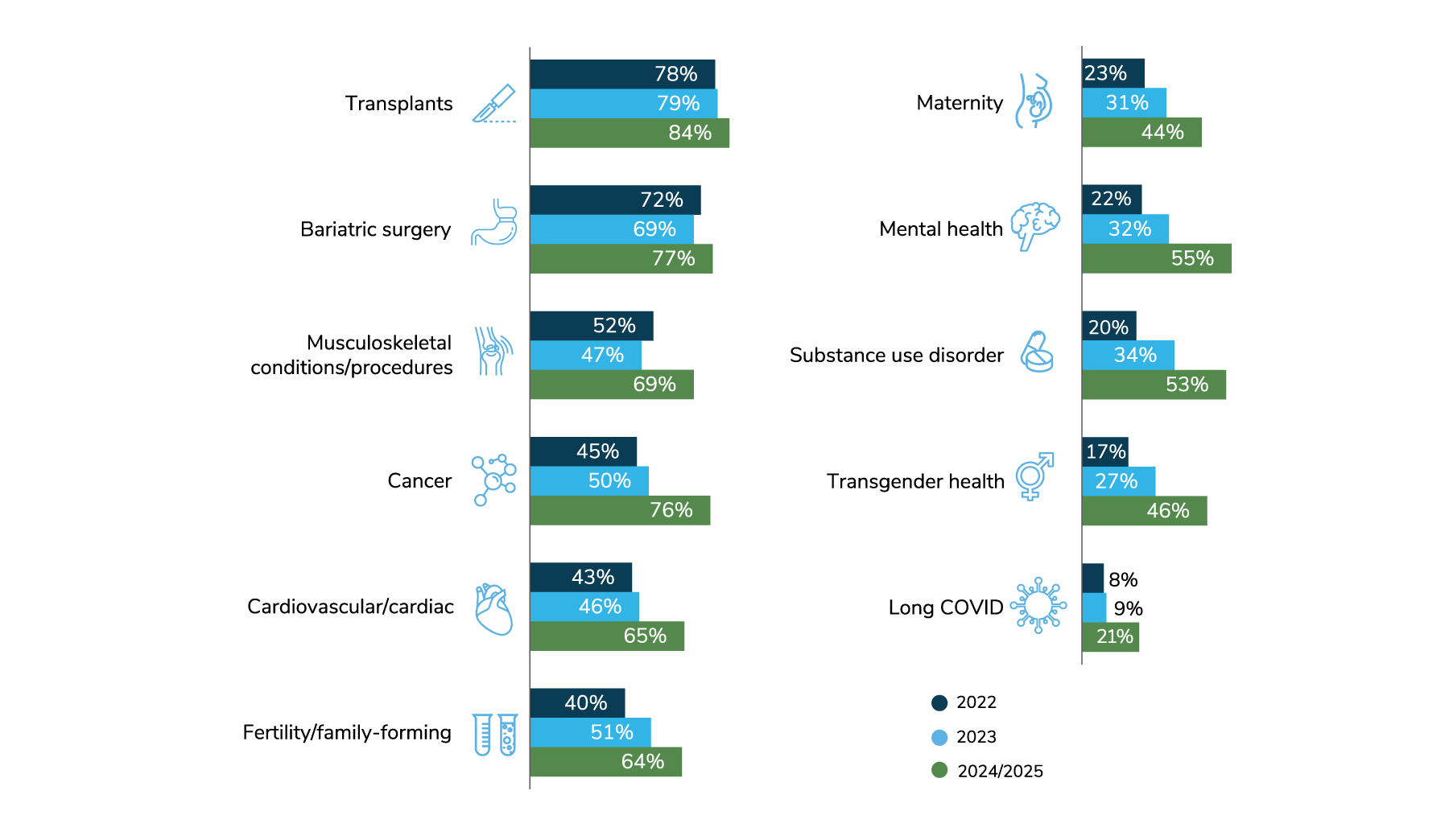
Source: 2023 Large Employers’ Health Care Strategy and Plan Design Survey
How Do COEs Fit Into a Value-Based Care Strategy?
Patients are sent to COEs for individual procedures and episodes of care. The performance of a COE and related payments are often based on individual patient outcomes (e.g., cancer treatment) or procedures (e.g., bariatric surgery or transplants.) A geographically disbursed employer with or without a strong opportunity for population- level value-based arrangements may still want to pursue a COE strategy given the high-cost nature of many conditions they treat and the ability to support short-term travel for individual procedures.
Many employers have both COEs and population-level value-based arrangements. In these cases, negotiation between the health plan or accountable care organization (ACO) is necessary to determine whether care delivered by the COE will be included in the overall cost calculation that ACOs, high-performance networks (HPNs) or primary care providers are held accountable for. Providers held accountable for the total cost of care for their attributed population usually want to do as much of the care for their patients as they can to maintain control over that care, even if a COE with excellent results may be able to achieve superior outcomes.
How Are COEs Reimbursed?
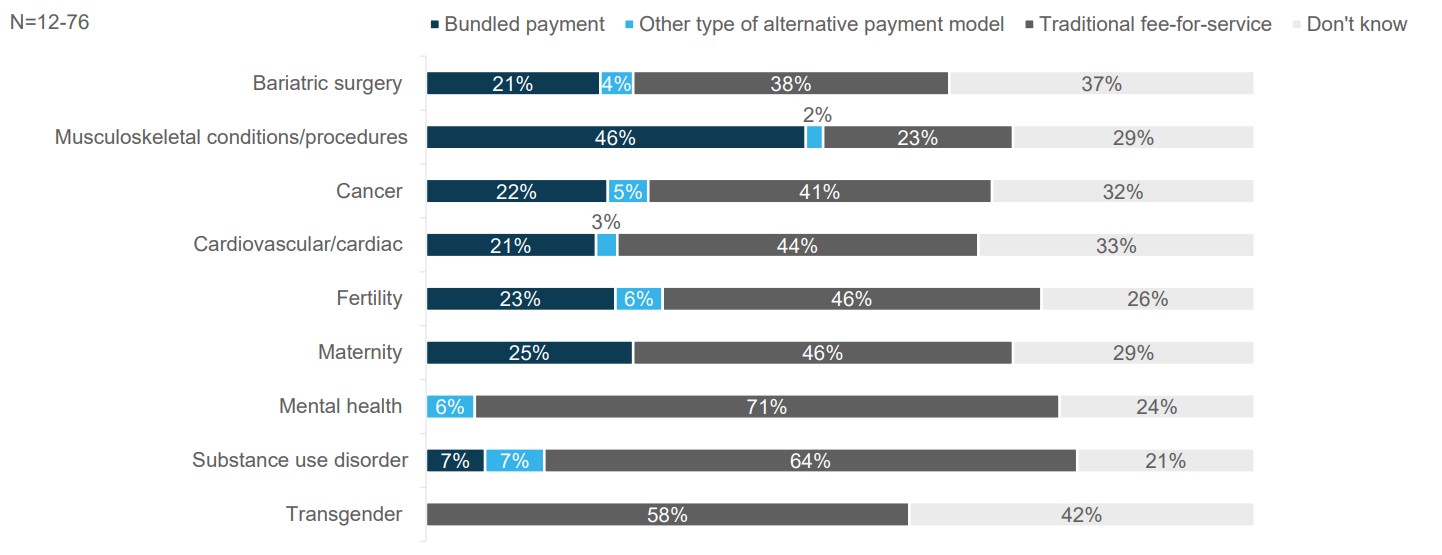
Source: 2021 Large Employers’ Health Care Strategy and Plan Design Survey
Most COEs are still reimbursed based on fee-for-service (FFS) payments but must maintain very high- quality and outcomes metrics to remain in an employer or health plan’s COE network. Akin to high-performance networks, while the reimbursements for COEs under FFS are not necessarily value-based, the requirements for providers to retain high-quality, strong outcomes and patient experience scores warrant the inclusion of COEs paid by FFS in a discussion of value-based care strategies.
A smaller but significant portion of COEs is reimbursed through bundled payments that incentivize coordination of care with community providers and create additional predictability in costs over time. See Part 2: Payment Models to learn more about how bundled payments are structured and how they can be used for COEs.
Conclusion
COEs are an excellent strategy for employers looking to optimize care for a particular type of procedure or condition. Many of them accept value-based reimbursements and must have very high standards for quality and outcomes in order to be designated as COEs. For discrete, time-limited services, COEs are an excellent strategy for employers who have other value-based arrangements in certain markets and for those who do not.
Employer Recommendations
- 1 | Assess your claims data to identify high-cost procedures or conditions for which a COE may be most impactful for your plan members. Focus your efforts on identifying COEs that provide those services and determining how value-based reimbursements can be incorporated into COE contracts to further tie the quality of the provider and outcomes to reimbursement.
- 2 | Ask health plans for outcomes and cost of care for your target procedures or conditions across your standard PPO networks, as well as in the COEs they contract with. Ask for the reimbursement arrangements used for these COEs.
- 3 | Decide what level of excellent outcomes, cost of care and value-based arrangements are necessary from a COE to consider steering your employees to those providers. COEs should have significantly greater outcomes compared to the rest of the PPO networks; many health plans and employers assess the percentile of performance a potential COE is delivering compared to other providers. A provider that is in the top quartile or decile of performance on both quality and efficiency metrics may be appropriate for a COE designation, depending on employers’ standards for inclusion.
- 4 | Consider reducing cost-sharing and offering travel benefits for employees using COEs that accept value-based reimbursements. COE providers that enter into value-based reimbursement arrangements may negotiate for some amount of “steerage” to their centers in exchange for their willingness to take on financial risk.
For a more detailed list of recommendations, see the Business Group’s Centers of Excellence Considerations for Employers.
More Topics
Articles & Guides- 1 | Centers for Medicare & Medicaid Services. Performance Year 2021 APM Performance Pathway: CMS Web Interface Measure Benchmarks for ACOs. Quality Payment Program. Accessed October 11, 2022. https://qpp-cm-prod-content.s3.amazonaws.com/uploads/1306/Performance%20Year%202021%20APM%20Performance%20Pathway-CMS%20Web%20Interface%20Measure%20Benchmarks%20for%20ACOs.pdf
- 2 | The Leapfrog Group. Preventing and Responding to Patient Harm. Leapfrog Ratings. Accessed October 11, 2022. https://ratings.leapfroggroup.org/measure/hospital/preventing-and-responding-patient-harm
- 3 | Agency for Healthcare Research and Quality. About CAHPS. July 2022. Accessed October 11, 2022. https://www.ahrq.gov/cahps/about-cahps/index.html
- 4 | Conti R et al. Projections of US Prescription drug spending and key policy implications. JAMA Health Forum. 2021;2(1). https://jamanetwork.com/journals/jama-health-forum/fullarticle/2776040. Accessed November 8, 2022.
- 5 | Business Group on Health. Emerging Trends in Cancer Care. October 25, 2021. https://www.businessgrouphealth.org/resources/emerging-trends-in-cancer-care. Accessed November 8, 2022.
- 6 | Golden W et al. Changing how we pay for primary care. New England Journal of Medicine Catalyst. November 20, 2017. https://catalyst.nejm.org/doi/full/10.1056/CAT.17.0326. Accessed November 8, 2022.
- 7 | Bitton A et al. Off the hamster wheel? Qualitative evaluation of a payment-linked patient-centered medical home (PCMH) pilot. The Milbank Quarterly. 2012 Sep; 90(3): 484–515. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3479381/. Accessed November 8, 2022.
- 8 | Primary Care for Boeing’s Mesa Employees. Iora Health. Accessed on February 9, 2022. https://ioraprimarycare.com/boeing/
- 9 | Bleser W, et al Half a decade in, Medicare accountable care organizations are generating net savings: Part 1. Health Affairs Blog. September 20, 2018. https://www.healthaffairs.org/do/10.1377/forefront.20180918.957502/full/. Accessed November 8, 2022.
- 10 | Sullivan G, Feore J. Physician-led accountable care organizations outperform hospital-led counterparts. Avalere. October 15, 2019. https://avalere.com/press-releases/physician-led-accountable-care-organizations-outperform-hospital-led-counterparts. Accessed November 8, 2022.
- 11 | Business Group on Health. 2023 Large Employers’ Health Care Strategy and Plan Design Survey. https://www.businessgrouphealth.org/resources/2023-plan-design-health-care-delivery-system. Accessed November 8, 2022.
- 12 | Lapsey H. The Better Benefit Stack. 2018 Oliver Wyman Health Innovation Journal. https://health.oliverwyman.com/2019/03/the-better-benefit-stack.html
- 13 | Centers for Medicare & Medicaid Services. Medicare Shared Savings Program Continues to Grow and Deliver High-Quality, Person-Centered Care Through Accountable Care Organizations. CMS Newsroom. January 26, 2022. https://www.cms.gov/newsroom/press-releases/medicare-shared-savings-program-continues-grow-and-deliver-high-quality-person-centered-care-through. Accessed November 8, 2022.
- 14 | O’Reilly K. Doctor participation in ACOs, medical homes grows amid pandemic. American Medical Association. December 7, 2021. https://www.ama-assn.org/practice-management/payment-delivery-models/doctor-participation-acos-medical-homes-grows-amid. Accessed November 8, 2022.
- 15 | Avalere. MSSP Sees Continued Growth in Downside Risk ACOs. January 21, 2020. https://avalere.com/insights/mssp-sees-continued-growth-in-downside-risk-acos. Accessed November 8, 2022.
- 16 | Mechanic R et al. The 2018 Annual ACO Survey: Examining the Risk Contracting Landscape. Health Affairs Forefront. April 23, 2019. https://wwwhealthaffairs.org/do/10.1377/forefront.20190422.181228/full/. Accessed November 8, 2022.
- 17 | Business Group on Health. 2023 Large Employers’ Health Care Strategy and Plan Design Survey. https://www.businessgrouphealth.org/resources/2023-large-employers-health-care-strategy-and-plan-design-survey
- 18 | Business Group on Health. 2023 Large Employers’ Health Care Strategy and Plan Design Survey. https://www.businessgrouphealth.org/resources/2023-plan-design-health-care-delivery-system.
- 19 |Elkins K. Lowe's free surgery program helps cut costs, benefit employees. Charlotte Business Journal. March 30, 2016. https://www.bizjournals.com/charlotte/blog/outside_the_loop/2016/03/lowe-s-free-surgery-program-helps-slice-costs.html. Accessed November 8, 2022.
-
IntroductionValue-based Purchasing Employer Guide: Introduction
-
Executive SummaryValue-based Purchasing Employer Guide: Executive Summary
-
Part 1Definitions and Measures of Value in Value-based Purchasing
-
Part 2Value-based Reimbursement Strategies
-
Part 3Value-based Primary Care
-
Part 4Accountable Care Organizations and High-Performance Networks
-
Part 5Centers of Excellence
-
Part 6Value-based Virtual Care
-
Part 7Value-based Care Engagement Strategies
This content is for members only. Already a member?
Login
![]()
