November 27, 2023
Advancements in genetic testing and therapies have required both health plans and providers to expand their services. They also have resulted in the creation of new types of partners whom employers can engage with for more support in navigating this complex field. The new classes of service providers can also assist doctors, health plans and patients in appropriately utilizing genetic testing, treatments and interpreting the data. Opportunities may arise for employers to engage with these vendors to manage cost and utilization.
Some Key Players in Precision Medicine
- Providers: Prescribe tests for patients, collect genetic material– and help patients interpret the results. Genetic testing and treatments are typically ordered by geneticists but can also be ordered and prescribed by primary care providers, oncologists and other specialists.
- Genetic Counselors: Genetic counselors have advanced training in medical genetics and counseling and guide patients seeking more information about how inherited diseases and conditions might affect them or their families. Genetic counselors can help both patients and providers choose the right tests and interpret test results. There are a little over 6,500 licensed genetic counselors in the U.S., and the field is rapidly growing, largely due to growth in the development of genetic tests has created higher demand for both tests and for counselors.11 Some of the new players within precision medicine include virtual genetic counseling companies.
- Lab Testing Companies: Process genetic material delivered to them by providers. There are hundreds of labs across the country that run tests and submit claims to health plans.
- Health Plans: Set medical policy and coverage guidelines and execute prior authorizations for genetic testing and gene therapies.
- Lab Benefit Managers (LBMs): Manage the laboratory testing benefit for payers. Given the complexity and evolving landscape, even major health plans need outside support to manage genetic testing utilization, prior authorization and lab claims.
- Genetic Benefit Managers: Offer comprehensive end-to-end programmatic solutions related to genetic testing and management of genetic test and therapy benefits. Their primary goal is to assist patients, but they may also adopt some functions of LBMs
- Pharmaceutical Companies: Develop gene therapies for administration by expertly trained providers. They also often launch such therapies with companion genetic tests that help determine if the drug will be effective in particular patients based on their genetics.
- Direct-to-Consumer Testing (DTC) Companies: Sell genetic tests directly to consumers, who can send saliva samples directly to the company for processing. These DTC companies also sell to employers.
- Patients: They are, of course, the reason for these new treatments and tests. Patients are affected by decisions made by each of these key players, often while navigating diagnosis and treatment journeys of their own, which can be frightening and expensive.
LBMs: The New Addition to the Alphabet Soup of Health Care Industry
Similar to how pharmacy benefit managers (PBMs) emerged in the wake of rising pharmacy costs, laboratory benefit managers (LBMs) are a new type of benefit manager being contracted by employers and/or insurers to help lower costs and enhance quality of care through lab utilization management practices.12 The need is clear, as laboratory tests represent the most common medical procedure. Even before the need for COVID-19 testing arose, labs were vital in assisting health care providers and patients with monitoring, diagnosing and treating disease. Their role is to perform a wide range of services, from routine blood tests to groundbreaking genetic and molecular tests. In 2019, over 7 billion lab tests were performed in the U.S.13 In fact, prior to the COVID-19 pandemic, genetic testing, was the fastest growing area of laboratory tests.
The scope of services offered by LBMs may include:
- Developing prior authorization requirements and performing prior authorizations;
- Developing preferred lab and provider networks to manage cost and quality of lab testing;
- Developing test formularies for payers to reduce inappropriate testing;
- Utilization management and assisting payers with medical necessity review;
- Lab claim processing and reviews;
- Developing coverage policies; and
- Monitoring emerging evidence and the new testing landscape for timely updates to coverage policies. Some LBMs may describe their basis for developing coverage policies and make such policies publicly available, making it transparent to patients and payers that such coverage decisions are rooted in clinical evidence.
The Importance of Genetic Counseling
Patients may be referred to a genetic counselor by their doctor (such as an obstetrician, oncologist or medical geneticist) to discuss their family history and genetic risks, or before or after having genetic testing. For some patients, genetic counselors should be an integral part of their health care team.
Their role is to help patients understand:
- Genetic risks based on family history;
- Genetic risks for certain diseases or cancer;
- Whether genetic testing might be right for them; and
- What the results of genetic tests may mean for both patients and their families.
Genetic counselors can also provide emotional support and assist with shared decision making by empowering patients and equipping them with relevant and clinically accurate information.11
Genetic Benefit Managers: Bringing Genetic Expertise to the Continuum of Genetic Benefit Management
In 2022, the genetic testing market surpassed $18 billion and is expected to climb as high as $43 billion by 203254 The complexity associated with the administration and design of genetic test benefits has sparked the creation of companies specializing in genetic benefits management, some of which are contracting with health plans, LBMs or directly with employers.
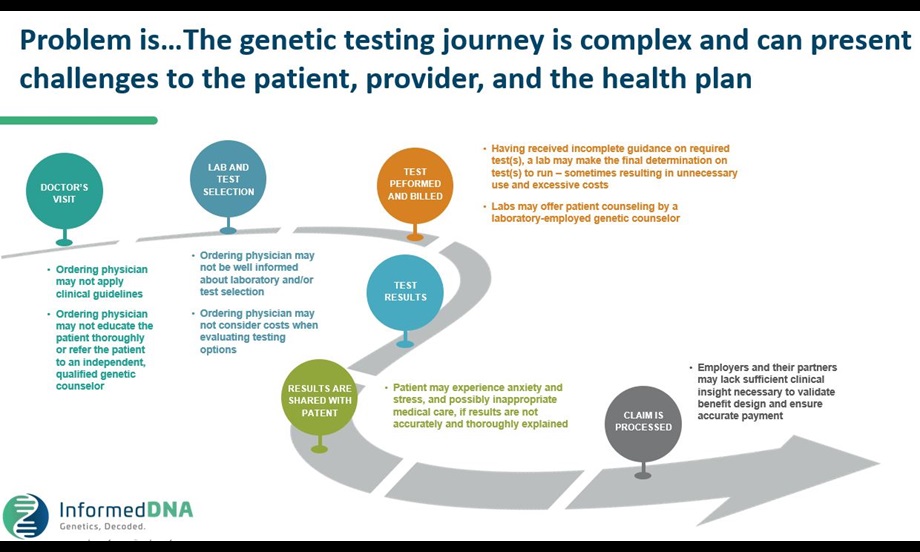
Genetic benefit managers claim to offer end-to-end solutions that assist consumers but may also adopt some functions of LBMs. The scope of their services may include:
- Genetic counseling and risk assessment for patients, often through virtual platforms;
- Engagement of credentialed genetics specialists to assist providers without genetic expertise with test selection and risk assessment, augmenting the ordering providers’ genetic knowledge with real time online clinical review;
- Assisting patients directly with genetic test selection;
- Managing the preauthorization process for genetic testing;
- Assisting patients and providers in interpreting genetic test results;
- Developing genetic test coverage policy; and
- Ensuring claim payment integrity and quality through genetic test claims analytics and audits.
In addition to LBMs and genetic benefit managers, there is a growing class of companies marketing genetic tests directly to consumers and employers. Such companies serve as intermediaries between consumers and physicians prescribing genetic tests, which can mean that patients never actually meet the physicians. Instead, the company requests a physician’s order after the consumer purchases a test online. Some observers have noted that this practice is an example of the testing landscape outpacing the current regulatory framework by circumventing the involvement of physicians in ordering and interpreting genetic test results.14
Conclusion
Employers considering engaging with new partners for better management of the genetic benefit should evaluate the landscape of providers of such services, understand their relationships with health plans and PBMs and look for potential synergies in engaging with those already affiliated with existing partners. Reviewing existing genetic claim data may help employers assess the needs of their population. Timely engagement with experts may benefit employers by creating the proper framework for genetic testing coverage and review to prepare them for the inevitable continued expansion of testing costs and utilization.
More Topics
Articles & Guides- 1 | National Institutes of Health. NIH Fact Sheets. Genetic Testing: How It Is Used for healthcare. June 30, 2018. https://archives.nih.gov/asites/report/09-09-2019/report.nih.gov/nihfactsheets/ViewFactSheetef83.html. Accessed December 2, 2020.
- 2 | Halbisen AL, Lu CY. Trends in Availability of Genetic Tests in the United States, 2012-2022. J Pers Med. 2023;13(4):638. Published 2023 Apr 6. doi:10.3390/jpm13040638. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10142561/. Accessed September 20, 2023.
- 3 | U.S. Food & Drug Administration. Approved Cellular and Gene Therapy Products. June 30, 2023. https://www.fda.gov/vaccines-blood-biologics/cellular-gene-therapy-products/approved-cellular-and-gene-therapy-products. Accessed September 20, 2023.
- 4 | Hunt, T. The Cell And Gene Therapy Sector in 2023: A Wave Is Coming - Are We Ready? January 9, 2023. https://invivo.pharmaintelligence.informa.com/IV146781/The-Cell-And-Gene-Therapy-Sector-In-2023-A-Wave-Is-Coming--Are-We-Read. Accessed September 23, 2023.
- 5 | Business Group on Health. 2024 Large Employer Health Care Strategy Survey. August 22, 2023. https://www.businessgrouphealth.org/resources/2024-large-employer-health-care-strategy-survey-intro. Accessed September 20, 2023.
- 6 | Informed DNA. Cost & Delivery Institute Presentation: Genetic Benefits Management: Best Practices. January 22, 2020.
- 7 | Hauser D, Obeng A, Fei K et al. Views of primary care providers on testing patients for genetic risks for common chronic diseases. Health Affairs. 2018 May;37(5):793-800. https://www.healthaffairs.org/doi/10.1377/hlthaff.2017.1548. Accessed December 5, 2020.
- 8 | Brodwin E. After you spit into a tube for a DNA test like 23andMe, experts say you shouldn’t assume your data will stay private forever. Business Insider. February 16, 2019. https://www.businessinsider.com/privacy-security-risks-genetic-testing-23andme-ancestry-dna-2019-2. Accessed December 5, 2020.
- 9 | Hendricks-Sturrup R, Prince AER, Lu CY. Direct-to-consumer genetic testing and potential loopholes in protecting patient privacy and nondiscrimination. JAMA. 2019, 32(19): 1869-1870.https://jamanetwork.com/journals/jama/fullarticle/2731672?widget=personalizedcontent&previousarticle=2706179. Accessed December 5, 2020.
- 10 | Medline Plus. Genetic Testing. September 10, 2020. https://medlineplus.gov/genetics/understanding/testing/. Accessed December 5, 2020.
- 11 | National Society of Genetic Counselors. 2023 Professional Status Survey. 2023. https://www.nsgc.org/Portals/0/2023%20PSS%20Executive%20Summary.pdf. Accessed September 20, 2023.
- 12 | Phillips KA, Deverka PA. The emerging use by commercial payers of third-party lab benefit managers for genetic testing. Health Affairs Blog. October 23, 2019. https://www.healthaffairs.org/do/10.1377/hblog20191021.563154/full/. Accessed December 5, 2020.
- 13 | American Clinical Laboratory Association. Economic Impact of Clinical Labs. https://www.acla.com/economic-impact-of-clinical-labs/. Accessed December 5, 2020.
- 14 | Swetlitz I. Genetic tests ordered by doctors race to market, while ‘direct-to-consumer’ tests hinge on FDA approval. STAT. March 16, 2018. https://www.statnews.com/2018/03/16/genetic-tests-fda-regulation/. Accessed December 5, 2020.
- 15 | Phillips KA, Deverka PA, Hooker GW et al. Genetic testing availability and spending: Where are we now? Where are we going? Health Affairs. 2018 May; 37(5): 710-716. https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2017.1427. Accessed December 5, 2020.
- 16 | Healthcare Fraud Prevention Partnership. White Paper: Genetic Testing: Fraud, Waste & Abuse. July 2020. https://www.cms.gov/files/document/hfpp-genetic-testing-fwa-white-paper.pdf. Accessed December 5, 2020.
- 17 | National Cancer Institute at the National Institutes of Health. Multiple-gene panel test. https://www.cancer.gov/publications/dictionaries/genetics-dictionary/def/multiple-gene-panel-test. Accessed December 5, 2020.
- 18 | American College of Obstetricians and Gynecologists (ACOG). Carrier Screening in the Age of Genomic Science. March 2017. https://www.acog.org/clinical/clinical-guidance/committee-opinion/articles/2017/03/carrier-screening-in-the-age-of-genomic-medicine. Accessed December 5, 2020.
- 19 | United States Preventive Services Task Force (USPSTF). Final Recommendation Statement: BRCA-Related Cancer: Risk Assessment, Genetic Counseling, and Genetic Testing. August 20, 2019. https://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/brca-related-cancer-risk-assessment-genetic-counseling-and-genetic-testing. Accessed July 8, 2020.
- 20 | Nelson HD, Huffman LH, Fu R, Harris EL, Walker M, Bougatsos C. Genetic risk assessment and BRCA mutation testing for breast and ovarian cancer susceptibility. Agency for Healthcare Research and Quality (US); September 2005. https://pubmed.ncbi.nlm.nih.gov/20722133/. Accessed December 5, 2020.
- 21 | American College of Obstetricians and Gynecologists (ACOG). Carrier Screening FAQs. October 2020. https://www.acog.org/patient-resources/faqs/pregnancy/carrier-screening. Accessed December 5, 2020.
- 22 | Molteni M. 23andMe’s new diabetes test has experts asking who it’s for. Wired. March 10, 2019. https://www.wired.com/story/23andmes-new-diabetes-test-has-experts-asking-who-its-for/. Accessed December 5, 2020.
- 23 | Catalyst for Payment Reform. How-to Guide: Unraveling Genetic Testing Benefits. December 2018. https://www.catalyze.org/product/value-genetic-testing-benefits/. Accessed December 5, 2020.
- 24 | Mayo Clinic. Pharmacogenomics Finding the Right Medication for You. 2013. https://mcforms.mayo.edu/mc1200-mc1299/mc1205-70.pdf. Accessed on December 5, 2020.
- 25 | Aon. Evidence-based Benefit Design Committee Presentation: Introduction to Human Genomics. February 13, 2019.
- 26 | Centers for Disease Control and Prevention (CDC). Mental Health Conditions: Depression and Anxiety. August 6, 2020. https://www.cdc.gov/tobacco/campaign/tips/diseases/depression-anxiety.html. Accessed December 5, 2020.
- 27 | Grohol JM. Gene testing for antidepressants & psychotropics: Not there yet. PsychCentral Blog. December 6, 2019. https://psychcentral.com/blog/gene-testing-for-antidepressants-psychotropics-not-there-yet/. Accessed December 5, 2020.
- 28 | Jørgensen JT, Hersom M. Companion diagnostics—a tool to improve pharmacotherapy. Ann Transl Med. 2016 Dec; 4(24): 482. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5233535/. Accessed December 5, 2020.
- 29 | U.S. Food & Drug Administration (FDA). Companion Diagnostics. December 7, 2018. https://www.fda.gov/medical-devices/vitro-diagnostics/companion-diagnostics. Accessed December 5, 2020.
- 30 | FDA. List of Cleared or Approved Companion Diagnostic Devices (In Vitro and Imaging Tools). November 16, 2020. https://www.fda.gov/medical-devices/vitro-diagnostics/list-cleared-or-approved-companion-diagnostic-devices-vitro-and-imaging-tools. Accessed December 5, 2020.
- 31 | Jørgensen JT. Companion & Complementary Diagnostics: Clinical and Regulatory Perspectives. Dx-Rx Institute Presentation at Workshop on Companion Diagnostics. January 31, 2017. https://biomarkers.dk/fileadmin/user_upload/Editor/Files/Niels/Biomarkers/events/Jan_2017/Jan_170127_-_Companion_and_Complemnetary_Diagnostics.pdf. Accessed December 5, 2020.
- 32 | Levy B. . Clinical Progress and Coverage Policies in Immuno-Oncology. Episode 1: Existing Treatment Landscape of Immunotherapies. July 28, 2016. https://www.ajmc.com/insights/clinical-progress-and-coverage-policies-in-immuno-oncology/distinguishing-between-companion-and-complementary-diagnostic-tests. Accessed December 5, 2020.
- 33 | Vassy JL, Bates D, Murray M. Appropriateness: A key to enabling the use of genomics in clinical practice? The American Journal of Medicine. 2016 Jun; 129(6): 551-553. https://www.amjmed.com/article/S0002-9343(16)30198-X/pdf. Accessed December 5, 2020.
- 34 | CDC. Genomics & Precision Health: Evaluating Genomic Tests. September 20, 2019. https://www.cdc.gov/genomics/gtesting/index.htm. Accessed December 5, 2020.
- 35 | Genomics Education Programme (NHS). What is NIPT? December 18, 2017. https://www.genomicseducation.hee.nhs.uk/blog/what-is-nipt/. Accessed December 5, 2020.
- 36 | National Human Genome Research Institute (NHGRI). Noninvasive Prenatal Genetic Testing. April 17, 2018. https://www.genome.gov/dna-day/15-ways/noninvasive-prenatal-genetic-testing. Accessed December 5, 2020.
- 37 | ACOG. Prenatal Genetic Screening Tests FAQs. October 2020. https://www.acog.org/patient-resources/faqs/pregnancy/prenatal-genetic-screening-tests. Accessed December 5, 2020.
- 38 | Medline Plus. Genetics. August 31, 2020. https://ghr.nlm.nih.gov/primer/newbornscreening/nbscost . Accessed December 8, 2020.
- 39 | Mayo Clinic. Genetic Testing. https://www.mayoclinic.org/tests-procedures/genetic-testing/about/pac-20384827. Accessed December 5, 2020.
- 40 | American Association for the Advancement of Science (AAAS). Research supports expanding insurance coverage of non-invasive prenatal testing. Press Release. October 8, 2019. https://www.eurekalert.org/pub_releases/2019-10/uoca-rse100819.php. Accessed December 5, 2020.
- 41 | United Healthcare. Carrier Testing for Genetic Diseases – Commercial Medical Policy. Effective Date: July 1, 2020. https://www.uhcprovider.com/content/dam/provider/docs/public/policies/comm-medical-drug/carrier-testing-for-genetic-diseases.pdf. Accessed December 5, 2020.
- 42 | Cigna. Genetic Testing for Reproductive Carrier Screening and prenatal Diagnosis – Medical Coverage Policy. Effective Date: December 15, 2019. https://static.cigna.com/assets/chcp/pdf/coveragePolicies/medical/mm_0514_coveragepositioncriteria_genetic_testing_repro_carrier_prenatal.pdf. Accessed December 5, 2020.
- 43 | Rose S, Chun C. The test that saved my sister’s life and my own. Healthline Blog. July 27, 2020. https://www.healthline.com/health/breast-cancer/brca-gene-test-saved-my-life. Accessed December 5, 2020.
- 44 | Filipski KK, Mechanic LE, LongR et al. Pharmacogenomics in oncology care. Front Genet. 2014; 5:73. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3986526/. Accessed December 5, 2020.
- 45 | U.S. National Library of Medicine. ClinicalTrials.gov. 2020. https://clinicaltrials.gov/ct2/results?term=%22gene+therapy%22+OR+%22gene+transfer%22+OR+%22virus+delivery%22&Search=Apply&recrs=b&recrs=a&age_v=&gndr=&type=&rslt=. Accessed December 5, 2020.
- 46 | Blue Cross Blue Shield Association (BCBSA). Evidence-based Benefit Design Committee Presentation: Genetic Testing in Precision Medicine Presentation. February 13, 2019.
- 47 | McCray PB Jr. Difficulties of gene therapy. The Lancet Supplement. 2001 https://www.thelancet.com/pdfs/journals/lancet/PIIS0140673601070325.pdf. Accessed December 5, 2020.
- 48 | Rockoff JD. The million-dollar cancer treatment. Who will pay? The Wall Street Journal. April 26, 2018. https://www.wsj.com/articles/the-million-dollar-cancer-treatment-no-one-knows-how-to-pay-for-1524740401. Accessed December 5, 2020.
- 49 | LifeSciencesIntelligence. The Top 5 Most Expensive FDA-Approved Gene Therapies. May 24, 2023. https://lifesciencesintelligence.com/features/the-top-5-most-expensive-fda-approved-gene-therapies#:~:text=Zolgensma%2C%20and%20Luxturna.-,Hemgenix,as%20congenital%20factor%20IX%20deficiency. Accessed September 20, 2023.
- 50 | FDA. Statement from FDA Commissioner Scott Gottlieb, M.D. and Peter Marks, M.D., Ph.D., Director of the Center for Biologics and Evaluation and Research on new policies to advance development of safe and effective cell and gene therapies. January 15, 2019.https://www.fda.gov/news-events/press-announcements/statement-fda-commissioner-scott-gottlieb-md-and-peter-marks-md-phd-director-center-biologics. Accessed December 5, 2020.
- 51 | American Society of Gene & Cell Therapy. Annual meeting.ASGCT - American Society of Gene & Cell Therapy | ASGCT - American Society of Gene & Cell Therapy. Accessed December 8, 2020.
- 52 | Buckles S. Gene therapy: Potential and pitfalls. Mayo Clinic blog. November 19, 2018. https://individualizedmedicineblog.mayoclinic.org/2018/11/19/gene-therapy-potential-and-pitfalls/. Accessed on December 5, 2020.
- 53 | Business Group on Health. Quick Survey: Genetic Testing Benefit Offering. February 21, 2020. https://www.businessgrouphealth.org/resources/genetic-testing-benefit-offerings-quick-survey. Accessed December 5, 2020.
- 54 | Ugalmugle S, Swain R. Genetic Testing Market Size by Test Type (Predictive Testing, Carrier Testing, Prenatal and New-born Testing, Diagnostic Testing, Pharmacogenomic Testing, Nutrigenomic Testing), By Application (Cancer, Genetic Disease, Cardiovascular Disease), Industry Analysis Report, Regional Outlook, Application Potential, Competitive Market Share & Forecast, 2020 – 2026. Global Market Insights. February 2020. https://www.gminsights.com/industry-analysis/genetic-testing-market. Accessed December 5, 2020.
-
IntroEmployers’ Guide to Precision Medicine: Genetic Testing, Treatments and Implications for Coverage
-
Section 1Genetic Testing and Treatments: Key Challenges and Recommendations for Employers
-
Section 2Genetic Counseling and Benefit Management: New Partnerships Emerge
-
Section 3Genetic Testing Landscape
-
Section 4Key Applications of Genetic Testing in Reproductive Health and Oncology
-
Section 5Gene Therapy: Key Considerations for Employers
-
Section 6Deep Dive into Pharmacogenomics: Deploying Precision Medicine in Drug Prescribing
This content is for members only. Already a member?
Login
![]()
